Exploring near-death experiences (NDEs) in critical care settings always fascinates me, especially because these stories come from people who were literally at the edge of life. Many share strange and powerful moments that can totally reshape how they look at life, death, and even their own recovery. I want to share what I’ve learned about interesting outcomes people have reported during or after critical care NDEs, and why these moments leave a mark, both personally and in the medical world.

What Are NDEs in Critical Care?
Near-death experiences pop up in all kinds of medical emergencies, but they’re pretty often reported in intensive care units (ICUs) where patients face life-threatening events. An NDE refers to a personal experience associated with death or impending death. Sometimes, folks remember leaving their body, seeing a tunnel, bright lights, or even meeting deceased loved ones. These aren’t just wild tales; surveys show about 10–23% of people who survive a cardiac arrest in the hospital mention some NDE-like recollections.
The chart below shows a few common NDE features and how often people report them after surviving a critical care episode:
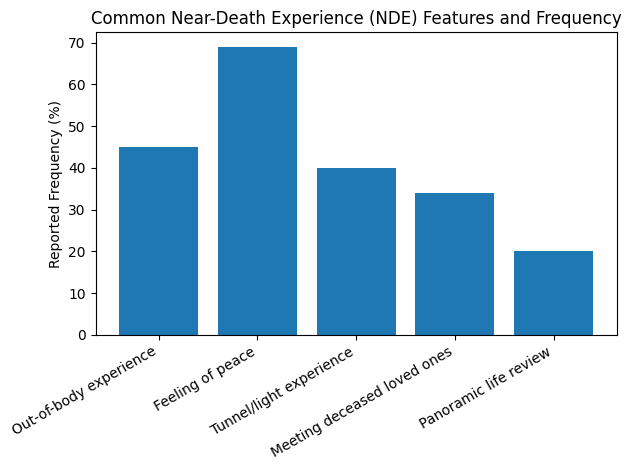
Source: Peer-reviewed survey data compiled from critical care and cardiology studies (see National Institutes of Health for details).
Typical Critical Care Scenarios Leading to NDEs
ICUs are high stress places where the difference between life and death can be measured in moments. Most NDEs in these environments happen during cardiac arrest, severe sepsis, respiratory failure, trauma, or complications from surgery. I’ve heard many stories from healthcare workers describing patients who wake up and recount vivid experiences, even if their heart was stopped or brain activity was nearly flat.
- Cardiac Arrest: Most research into NDEs comes from cardiac arrest survivors. A person’s heart stops, they lose pulse, and brain function drops sharply. Yet some wake up with memories of events while they were technically “gone.”
- Respiratory Failure: Severe breathing issues requiring intubation and ventilation can also trigger NDE reports.
- Multiorgan Failure: Complicated cases, especially in older adults, can push the body to its limits, and some people return with stories they remember clearly.
Critical care teams are often surprised by the clarity and detail in these accounts. Sometimes, survivors describe conversations or details from the time they were unresponsive, which puzzles even experienced staff. This curiosity has driven more systematic study of NDEs in ICU settings. It highlights how these episodes are not limited to a single diagnosis or demographic, but instead can affect anyone in crisis.
Fascinating Psychological and Emotional Changes After NDEs
One thing that really stands out is how an NDE can change someone’s life. Beyond the wild visions or sensations, people say their outlook on life actually brightens up.
Based on interviews and published research, here are some typical psychological and emotional outcomes noted in critical care NDE survivors:
| Reported Change | Short Description |
|---|---|
| Less fear of death | People commonly lose their anxiety about dying |
| Greater appreciation of life | Everyday events feel more meaningful |
| Personality transformation | More empathy, patience, or tolerance reported |
| Difficulty relating to others | Some feel isolated or misunderstood by family or friends |
| Boost in spirituality | Interest in spiritual or existential ideas increases |
These changes aren’t just in people’s heads, they’ve been documented in follow-up surveys as lasting for months or even years after an ICU discharge. Family members sometimes notice their loved one comes back with a totally different perspective on daily life or relationships. Even healthcare workers who witness these transformations often say that NDEs give survivors a new sense of gratitude or purpose. Some report newfound creativity or a stronger desire to give back to their community. It’s not unusual for people to seek out new hobbies, switch jobs, or reinvent their boundaries with friends and family as a result of their experience.
How Critical Care Teams Respond to NDE Reports
Doctors and nurses in the ICU are trained for physical emergencies, but stories of NDEs don’t always fit the usual workflow. I’ve found that reactions among staff can range from supportive and curious to skeptical or uncomfortable. Still, studies show that when medical teams treat patient recollections seriously, survivors feel much more supported in their recovery.
Some hospitals now provide training to help staff handle conversations about NDEs without judgment. This can lower distress for both patients and staff. Here’s a simple table showing steps clinical teams might use if a patient shares an NDE:
| Care Team Action | Benefit |
|---|---|
| Listening with empathy | Promotes trust and emotional healing |
| Validating experience | Reduces feelings of isolation |
| Referring to counseling/spiritual care | Encourages healthy processing of events |
Several studies support the idea that a supportive care team can help survivors feel safer discussing their experiences. Specialized counselors or chaplains may join the care process to help patients work through any troubling memories or existential questions tied to an NDE. In some cases, group sessions with other survivors can make it easier for individuals to share and process their stories, giving emotional healing a real boost.
Scientific Theories Behind NDEs in Critical Care
Lots of people wonder if there’s a scientific explanation behind NDEs. Right now, nobody has come up with one answer that covers every case, but a few theories are often discussed:
- Lack of Oxygen (Hypoxia): When the brain is short on oxygen, strange visions and sensations can happen. Some studies connect specific NDE images, like tunnels or bright lights, to the brain’s response to hypoxia.
- Chemical Changes: ICU drugs, body chemistry, or neurotransmitter shifts during trauma may play a role in creating vivid dreams or altered states.
- End of Life Brain Activity: Brain scans of dying patients sometimes show bursts of organized activity, even after the heart stops. This could trigger intense recollections or sensations.
- Psychological Coping: Facing extreme stress might prompt the mind to create comforting or meaningful experiences as a kind of self-defense.
No theory fully explains every element, especially when people report accurate awareness of events going on around them while unconscious. That’s why the medical world still finds NDEs kind of mysterious and worth more research. Some researchers point out the importance of cultural background, belief systems, and prior life experiences in shaping how these episodes are remembered and interpreted.
Real-Life Examples: Stories That Stick With Me
It’s easy to get caught up in theory, but personal stories really drive home why NDEs are such a hot topic in critical care. Here are a couple of patient experiences that I always find memorable:
- A patient revived after cardiac arrest reported “floating above” the ICU, watching staff work on their body, and later describing the exact layout of the room and overhead equipment.
- Another person recalled rushing through a dark tunnel toward a light, then meeting loved ones. After recovery, this patient said their lifelong fear of death had gone away completely.
- Some folks come back feeling like their purpose has changed and immediately take up new hobbies, relationships, or even switch careers.
Healthcare workers sometimes notice these shifts in patients after an NDE, like a deeper sense of calm or a new passion for helping others. For example, one nurse described a patient who, after a remarkable NDE, started volunteering at the hospital to support others going through critical illness. There’s more info and a whole database of shared NDE stories on the Near-Death Experience Research Foundation website.
Possible Challenges After a Critical Care NDE
Not every NDE has a purely positive outcome. Some survivors feel overwhelmed, isolated, or like their story isn’t taken seriously. This can add a layer of stress to recovery. Sometimes, people run into:
- Difficulty with friends/family: Loved ones may be skeptical, which can be frustrating or lonely for survivors.
- Nightmares or anxiety: NDEs can sometimes come with troubling memories or fear.
- Adjustment struggles: Major switches in worldview or personal values can create friction at work or in relationships.
Support groups, counseling, or connecting with others who’ve had NDEs can really help with these adjustments. Many hospitals now include post-discharge mental health evaluations for patients reporting NDEs, to smooth the way back to daily life. Online communities and peer support networks also offer valuable spaces for sharing experiences and advice on how to move forward after a life-changing event.
FAQs About NDEs in the ICU and Beyond
Here are a few questions I often get when chatting with people about near-death experiences, especially in a hospital setting:
Are NDEs proof of life after death?
NDEs are super interesting and big on personal meaning, but science hasn’t found clear proof they confirm anything about the afterlife.
Do all ICU survivors have NDEs?
Not at all. Most do not. But a notable percentage has some kind of strange sensory or emotional memory after intensive care.
Can medical teams learn from NDEs?
Absolutely. By listening and supporting patients who report NDEs, teams can help them adjust emotionally and promote better mental health after a critical illness.
Can NDEs affect physical recovery?
Sometimes, the psychological impact from an NDE (like less fear or a jump in optimism) can give patients a boost in motivation, potentially offering indirect benefits to their overall recovery and rehabilitation.
Do NDEs happen only in adults?
No, children in the ICU have also reported NDEs, although their stories might reflect their age or developmental stage. Experiences can be just as powerful or memorable as those reported by adults.
Final Thoughts
NDEs in critical care settings aren’t just stories. They’re experiences that can impact medical teams, patients, and even family members. For survivors, these moments can spark longtime changes in their outlook, personality, and relationships. For clinicians and researchers, they offer a unique window into how the brain and consciousness might work during moments of crisis. Staying open-minded and informed about these experiences helps everyone in the ICU get through tough moments with a little more understanding and support. The topic still leaves a lot of questions open for future research, but one thing’s for sure: the voices of survivors are an important part of the conversation about life and death in critical care.
